-
Call Now
1800-102-2727
Peristalsis: Types, Functions, Practice Problems and FAQs
We all like doing small activities or experiments, right? Especially in schools, teachers make us do a lot of fun games and exercises which make us love the subject more. Have you ever done this activity where you were asked to pass a stone through a rubber tube? If so, you might have noticed that every time you squeeze the section of the tube behind the stone, the stone will move forward.
A similar type of movement occurs in our food pipe as well. When we swallow food, a certain type of movement enables the food to pass through the food pipe. This movement also ensures that the food particle passes through the entire alimentary canal. This movement is known as peristalsis.
Fig: Movement of food in the alimentary canal
Now, you may be wondering from where this movement was initiated. Can we feel this movement? Is this a voluntary or involuntary movement?
Yes, this movement is initiated from the oesophagus as soon as food enters and is involuntary. Peristalsis can be described as a wavelike contraction that allows food and liquid to pass through the digestive tract. These contractions ensure that the food particle moves from the oesophagus to the stomach and from there to the small intestine eventually leading to the large intestine. Let’s understand peristalsis in depth with the help of this article.
Table of contents
- Peristalsis
- Esophageal peristalsis
- Intestinal peristalsis
- Ureteral peristalsis
- Reverse peristalsis
- Functions of peristalsis
- Practice Problems
- FAQs
Peristalsis
Peristalsis is the sequence of involuntary wavelike muscular contractions of the gut that pushes the luminal contents downward. It is produced by involuntary contraction of circular muscles which is preceded by the simultaneous contraction of the longitudinal muscles and relaxation of the circular muscles.
GIF: Peristalsis in oesophagus
Physiology of peristalsis
Once the food is swallowed, the oesophagus starts the peristaltic movement, which includes the reflexive activities of the longitudinal and circular muscles present at the digestive tract. Peristalsis occurs in the oesophagus, stomach, small intestine and large intestine. The bolus formed in the mouth moves in a chronological order, i.e. from the mouth to the oesophagus and then to the stomach, from there to the remaining parts of the GIT. Here, in the stomach, the food gets mixed with gastric juices and forms the chyme. Chyme then moves to the small intestine and where it mixes with the bile juice and intestinal juice or succus entericus. This then moves to the ileum, where nutrients are absorbed, as the digestion is completed. After digestion, it then passes to the large intestine and here, water is absorbed and the undigested food materials are temporarily stored in the rectum. From here it passed out of the body through the anus. Depending on the location of the gastrointestinal tract, these waves that move throughout the length of the GIT may be long, short, continuous, or intermittent.
Fig: Peristalsis helps in the movement of food in the alimentary canal
Types of peristalsis
Depending on the location of the peristalsis, it is of three types as follows:
- Esophageal peristalsis
- Intestinal peristalsis
- Ureteral peristalsis
Esophageal peristalsis
The contraction and relaxation of the muscles in the oesophagus or the food pipe forces the food down the track to the stomach, which is referred to as the esophageal peristalsis. Esophageal peristaltic waves begin in the upper part of the food pipe and then go to the entire length. The food particles that leave the oesophagus move with the help of secondary peristaltic waves and therefore, this wave removes leftover food particles. The whole circumference of the food pipe is covered by a single wave. After the stomach has been fully filled, the peristaltic waves disappear. Until gastric secretions dilute the food particles, these movements are halted. These waves assist in the proper blending of the contents of the stomach (food and gastric juice) and propel food into the small intestine. Two to three waves typically occur simultaneously in various parts of the stomach.
GIF: Peristalsis in oesophagus
Types of esophageal peristalsis
In the oesophagus, three types of peristalsis occurs as follows:
- Primary esophageal peristalsis
- Secondary esophageal peristalsis
- Tertiary esophageal peristalsis
Primary esophageal peristalsis
Primary esophageal peristalsis is initiated by the swallowing of food and is considered as the main source of esophageal transit. Primary esophageal peristalsis helps transfer food from the oesophagus into the stomach. It is a continuation of pharyngeal peristalsis and is controlled by the swallowing centre of the medulla oblongata and lower pons. It is prevented by vagotomy. Vagotomy is a surgical operation involving the cutting of one or more branches of the vagus nerve to reduce the rate of gastric secretions.
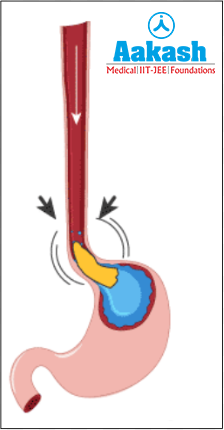
Fig: Primary esophageal peristalsis
Secondary esophageal peristalsis
Secondary esophageal peristalsis is also called the distension-induced peristalsis. It mainly functions to maintain an empty oesophagus by clearing refluxate from the stomach. If primary peristalsis is unable to convey the full bolus into the stomach, esophageal distention will start secondary esophageal peristalsis, which will continue until all of the contents are expelled. Different intraesophageal stimuli, such as air, mechanical distention, or water infusion, can physiologically cause secondary peristalsis. The efferent nervous system is involved in secondary peristalsis, which can function without the central nervous system input and continue to function after vagotomy.

Fig: Secondary esophageal peristalsis
Tertiary esophageal peristalsis
It is considered as the irregular contraction or indentations of the distal esophageal wall. The contractions seen here are isolated, simultaneous and dysfunctional. It is more common in older people. This normally occurs due to a motility disorder and can lead to impaired acid clearance. It is seen in Corkscrew oesophagus which results in diffuse esophageal spasm and achalasia oesophagus.
Regulation of esophageal peristalsis
The esophageal peristalsis is under the control of the following regions:
- Central and peripheral neural nervous system.
- Myenteric plexus
- Swallowing centre present in the lower pons and medulla oblongata.
- Extrinsic sympathetic and parasympathetic nerves.

Fig: Regulation of esophageal peristalsis
Intestinal peristalsis
The stimulation of the smooth muscle tissues present in the intestine is caused by the presence of food particles which will result in the contractions of the smooth muscles. These alternate wave-like contractions in the intestine are called the intestinal peristalsis. It helps in the proper mixing of food with digestive enzymes, and propulsion of the contents, at a proper rate to allow time for proper digestion and absorption of foods. These contractions also prevent overgrowth of bacteria in the intestine. Usually, these contractions are found in the small intestine and move in varying distances. Intestinal peristalsis occurs in two places as follows:
- Small intestine
- Large intestine
Peristalsis in the small intestine
A single peristaltic movement lasts only a few seconds as the chyme enters the small intestine. The chyme then moves at a speed of a few millimetres per second. The continuation of digestion and nutrient absorption is the main goal of the peristaltic movement in the small intestine. The food then passes from the small intestine to the large intestine after that.
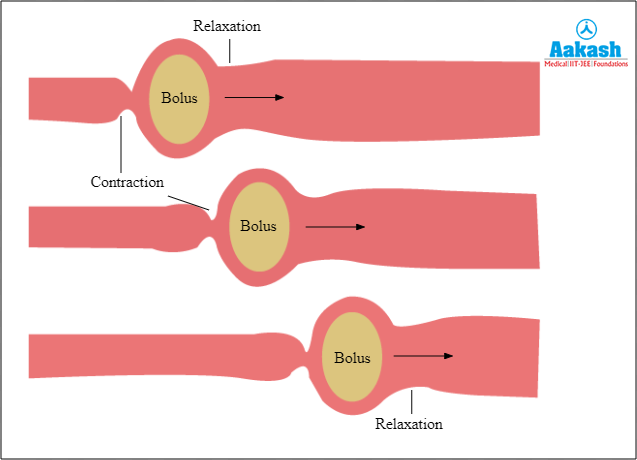
Fig: Peristalsis in the small intestine
Peristalsis in the large intestine
Similar to the small intestine, the large intestine also undergoes peristalsis. General contractions known as mass motions propel the digested food and happen one to four times per day. In order to be expelled from the gastrointestinal tract, faeces or other undigested waste materials are now moving in the direction of the rectum. The existence of chyme in the stomach and duodenum encourages these contractions, which are frequently brought on by meals.
Fig: Peristalsis in the large intestine
Regulation of intestinal peristalsis
The contractions of the smooth muscles of the gastrointestinal tract or GIT are controlled by many factors. It includes the following:
- Motor and sensory neurons
- Hormones like ghrelin (GHRL) and motilin (MLN) stimulate appetite and contractions.
- Contractility of the smooth muscles of the intestine.
Ureteral peristalsis
The peristalsis occurring in the urinary tract is called the ureteral peristalsis. It includes a series of compressive zones which correspond to waves of active muscular contractions that move at nearly constant speed along the ureter from kidneys towards the bladder. This causes the passage of urine from the kidneys to the urinary bladder. This peristalsis is triggered by calcium-dependent pacemaker cells present in the ureteral smooth muscles. Ureteral peristalsis increases infrequency and amplitude during obstructions. It also helps in the elimination of urine from the urethra through urinary orifice.

Fig: Regions of ureteral peristalsis
Regulation of ureteral peristalsis
The initiation and control of ureteral peristalsis is myogenic in nature. It depends on the activity of the pacemaker region in the renal pelvis. This region is under the influence of the rate of urine flow.
Reverse peristalsis
The wave-like muscle contractions of the gastrointestinal tract called peristalsis when moved backwards instead of forward. Then it is called antiperistalsis, reverse peristalsis or retroperistalsis. It occurs in the opposite direction of the typical peristaltic movement. This results in the contents of the gastrointestinal tract being forced to go backward. It normally happens prior to the action of vomiting. The emetic centre of the brain is activated by stomach irritation, particularly food poisoning or presence of bacteria signals an instant vomiting reflex, which results in the reverse peristalsis.

Fig: Reverse peristalsis
Reverse peristalsis in ruminants
The reverse peristalsis that brings the food back to the mouth for rechewing occurs in the case of ruminants like cattle (cows, oxen, bulls, or calves), sheeps, goats, giraffes, camels etc.

Fig: Ruminant
Regulation of reverse peristalsis
The vomiting centre is present in the fourth ventricle of the brain. The floor of the fourth ventricle contains an area called the chemoreceptor trigger zone (CTZ) or the area postrema. Stimulation of CTZ results in vomiting.
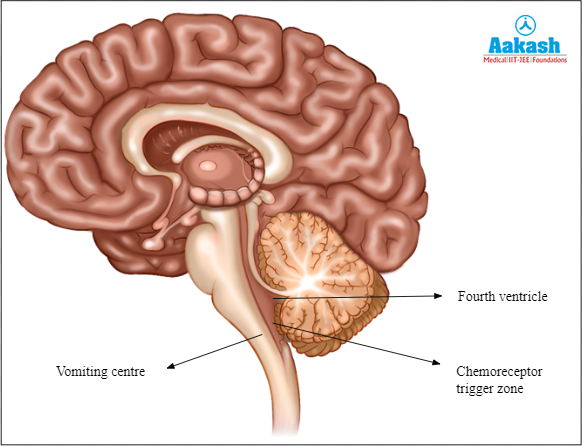
Fig: Regulating regions of reverse peristalsis
Mechanism of peristalsis
Through the myenteric plexus, the parasympathetic nervous system (PNS) stimulates peristalsis. The afferent (sensory) nerves of the myenteric plexus transmit data to interneurons inside the plexus. Interneurons interact with efferent (motor) nerves to cause smooth muscle cells to produce an action potential (spike-wave). This results in peristalsis.
The inner circular and outer longitudinal layers of muscle together are referred to as the muscularis propria which contains smooth muscle cells that are responsible for peristalsis. A bolus of food causes the intestines to stretch, which initiates reflexive stimulation of afferent neurons. The outer longitudinal muscles and inner circular muscles present just before the bolus contract in response to the efferent signal. This results in the shortening of the food tube and pushing the bolus forward. In addition, descending inhibitory reflexes force the circular muscles immediately behind the bolus to relax, allowing the bolus to move. Each peristalsis wave causes the bolus to migrate a few centimetres before the process starts all over again.
GIF: Mechanism of peristalsis
Stimulation of afferent nerves
The afferent nerves are stimulated via two types of mechanisms as follows:
- Reflexive (stretch or chemoreceptors)
- Parasympathetic stimulation (via acetylcholine)
Functions of peristalsis
The following are the major functions of peristalsis:
- It is the process by which muscular contractions aid food and liquid particles to move through the digestive tract.
- Food is pushed from the oesophagus into the stomach with the help of peristalsis.
- It helps in the formation of chyme by mixing the gastric juice and food particles.
- Peristalsis facilitates digestion by removing partially digested food from the small intestine.
- It also facilitates the circulation of nutrients from digested foods.
- These movements cause undigested waste materials to pass from the colon, into the rectum for temporary storage.
- It also helps in the expulsion of undigested waste materials from the body.
- The reverse peristalsis that brings the food back to the mouth for rechewing in cattle, sheep etc.
- Reverse peristalsis helps in the removal of unwanted substances from the body by vomiting.
- Peristalsis prevents overgrowth of bacteria in the intestine.
Practice Problems
- Peristalsis is the regular contraction and relaxation of muscles in the ____________.
a) Oesophagus
b) Buccal cavity
c) Alimentary canal
d) Stomach
Solution: Peristalsis is the sequence of involuntary wavelike muscular contractions of the alimentary canal that pushes the luminal contents downward. It is produced by involuntary contraction of circular muscles which is preceded by the simultaneous contraction of the longitudinal muscles and relaxation of the circular muscles. The contraction and relaxation of the muscles in the oesophagus or the food pipe forces the food down the track to the stomach, which is referred to as the esophageal peristalsis. Hence, the correct option is c.
2. What role does peristalsis play when it comes to digestion?
a) Breaking protein into amino acids
b) Breaking complex sugar into simple form
c) Easy assimilation of the food material
d) Smooth passage of food through the alimentary canal
Solution: Peristalsis is the sequence of involuntary wavelike muscular contractions of the alimentary canal that pushes the luminal contents downward. It is produced by involuntary contraction of circular muscles which is preceded by the simultaneous contraction of the longitudinal muscles and relaxation of the circular muscles. This uncontrollable movement is required for the smooth transportation of food through the oesophagus, stomach and intestine. It is also required to expel the undigested waste materials through the anus. Hence, the correct option is d.
3. In which of the following options, does peristalsis occur?
a) Throat
b) Windpipe
c) Oesophagus
d) Tongue
Solution: Peristalsis is the sequence of involuntary wavelike muscular contractions of the alimentary canal that pushes the luminal contents downward. It is produced by involuntary contraction of circular muscles which is preceded by the simultaneous contraction of the longitudinal muscles and relaxation of the circular muscles. The contraction and relaxation of the muscles in the oesophagus or the food pipe forces the food down the track to the stomach, which is referred to as the esophageal peristalsis. Hence, the correct option is c.
4. Mass peristalsis occurs in which part of the alimentary canal?
a) Stomach
b) Large intestine
c) Small intestine
d) Oesophagus
Solution: General contractions known as mass motions propel the undigested waste materials in the large intestine. It happens one to four times per day in the large intestine. In order to be expelled from the system, faeces or other undigested waste materials are now moving in the direction of the rectum. The existence of chyme in the stomach and duodenum encourages these contractions, which are frequently brought on by meals. Hence, the correct option is b.
FAQs
- In which area of the alimentary canal, the peristaltic waves are strongest?
Answer: Peristaltic waves begin as weak contractions at the beginning of the food pipe or oesophagus and gradually get stronger as they get closer to the distal stomach regions. The waves aid in blending stomach contents and pushing food to the small intestine.
Fig: Stomach
- Which type of food stimulates the process of peristalsis?
Answer: Magnesium induces peristalsis, making it a common component in laxatives. Beans, nuts, seeds, whole grains, and green leafy vegetables are all great sources of magnesium.
- Why is the colon responsible for constipation?
Answer: The stool travels through the colon too slowly when muscular contractions are slow or sluggish, which causes the colon to absorb too much water. Constipation happens when the colon absorbs too much water from the waste materials which dries out the stool. This makes it harder in consistency and difficult to push out of the body through the anus.
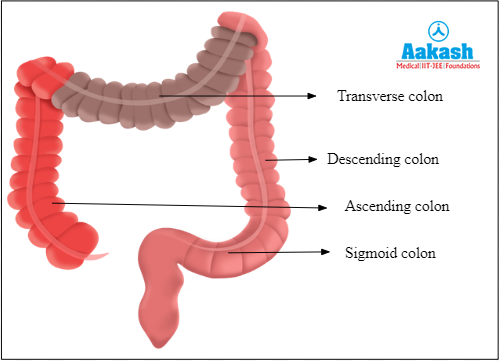
Fig: Colon
- Why does peristalsis weaken with age?
Answer: Peristalsis weakens with age and it is no longer triggered by each swallow. This is because both upper and lower esophageal sphincters lose tension. Moreover, the gag reflex is also absent in older people. Gag reflex or the pharyngeal reflex is considered as an involuntary reflex which involves the elevation of the soft palate and the bilateral pharyngeal muscle contraction.


