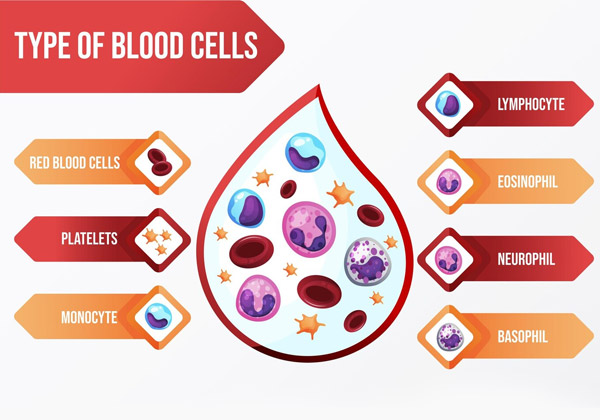
Blood is a vital fluid in the human body, essential for delivering nutrients, oxygen, and hormones to cells while removing waste products. It consists of a liquid component called plasma and three primary types of cells: Red Blood Cells (RBCs), White Blood Cells (WBCs), and Platelets. Each type of blood cell has unique characteristics and plays specific roles in maintaining health and supporting various physiological processes.
This comprehensive guide will explore these blood cells in detail, including their structure, functions, production, lifespan, and disorders.
Red Blood Cells (RBCs)
Structure and Composition of Red Blood Cells
Red Blood Cells (RBCs), also known as erythrocytes, are the most abundant type of blood cells. They are designed primarily for transporting oxygen from the lungs to the tissues and carbon dioxide from the tissues back to the lungs.
| Feature | Description |
| Shape | Biconcave disks |
| Size | Approximately 6-8 micrometers in diameter |
| Nucleus | Absent |
| Major Protein | Hemoglobin (iron-containing protein) |
| Primary Function | Oxygen transport from lungs to tissues and carbon dioxide transport from tissues to lungs |
The biconcave shape of RBCs increases the surface area for gas exchange and allows them to navigate through the smallest capillaries. The absence of a nucleus and other organelles provides more space for hemoglobin, which binds to oxygen and carbon dioxide.
Production and Lifespan
| Aspect | Description |
| Production Site | Bone marrow (through erythropoiesis) |
| Regulation | Hormone erythropoietin (produced by kidneys) |
| Average Lifespan | Approximately 120 days |
RBC production, or erythropoiesis, occurs in the bone marrow from hematopoietic stem cells. The process is regulated by erythropoietin, a hormone released by the kidneys in response to low oxygen levels. After approximately 120 days, aged RBCs are broken down by macrophages in the spleen, liver, and bone marrow.
Functions of Red Blood Cells
| Function | Description |
| Oxygen Transport | Hemoglobin binds oxygen in the lungs and delivers it to tissues. |
| Carbon Dioxide Transport | Hemoglobin also helps carry carbon dioxide from tissues back to the lungs. |
| pH Regulation | Hemoglobin acts as a buffer to help maintain blood pH. |
The primary role of RBCs is to transport oxygen and carbon dioxide. They also play a role in maintaining the pH balance of the blood by binding and releasing hydrogen ions.
Disorders of Red Blood Cells
| Disorder | Description | Symptoms |
| Anemia | Reduced number of RBCs or hemoglobin, leading to decreased oxygen-carrying capacity. | Fatigue, weakness, shortness of breath. |
| Polycythemia | Abnormal increase in RBC count, which can thicken the blood and increase the risk of clotting. | Risk of blood clots. |
Anemia can result from various causes, including iron deficiency, vitamin B12 deficiency, chronic diseases, and genetic disorders. Polycythemia can be primary (polycythemia vera) or secondary (due to chronic hypoxia or tumors producing erythropoietin).
White Blood Cells (WBCs)
White Blood Cells (WBCs), or leukocytes, are crucial for the immune system, defending the body against infections and diseases. They are categorized into two main groups based on the presence of granules in their cytoplasm: granulocytes and agranulocytes.
Granulocytes
| Type | Structure | Function |
| Neutrophils | Multi-lobed nucleus, granules | First responders to bacterial infections; phagocytosis. |
| Eosinophils | Bi-lobed nucleus, red-staining granules | Combat parasitic infections; involved in allergic responses. |
| Basophils | Bi-lobed or S-shaped nucleus, blue-staining granules | Release histamine and heparin; involved in allergic reactions. |
Granulocytes contain granules in their cytoplasm that are involved in their various functions. Neutrophils are the most abundant and respond quickly to infections. Eosinophils target parasitic infections and modulate allergic responses. Basophils are involved in inflammatory reactions by releasing substances like histamine.
Agranulocytes
| Type | Structure | Function |
| Lymphocytes | Large, round nucleus with thin cytoplasm | B cells produce antibodies, T cells destroy infected cells, NK cells target cancer cells. |
| Monocytes | Large, kidney-shaped nucleus | Differentiate into macrophages and dendritic cells; phagocytosis and antigen presentation. |
Agranulocytes lack visible granules and include lymphocytes and monocytes. Lymphocytes are essential for adaptive immunity, while monocytes differentiate into macrophages and dendritic cells, which play roles in phagocytosis and antigen presentation.
Production and Lifespan
| WBC Type | Production Site | Lifespan |
| Neutrophils | Bone marrow | Few hours to days |
| Eosinophils | Bone marrow | Few days |
| Basophils | Bone marrow | Few hours to days |
| Lymphocytes | Bone marrow (and lymph nodes) | Months to years |
| Monocytes | Bone marrow | Days to months |
WBCs are produced in the bone marrow and lymphoid organs. Their lifespans vary widely, with neutrophils having the shortest lifespan and lymphocytes potentially living for years.
Functions of White Blood Cells
| Function | Description |
| Immune Defense | Identify and destroy pathogens; initiate immune responses. |
| Inflammatory Response | Mediate inflammation to isolate and eliminate pathogens. |
| Allergy and Hypersensitivity | Respond to allergens and modulate immune responses. |
| Cancer Surveillance | Detect and destroy cancerous cells. |
WBCs play roles in both the innate and adaptive immune responses, helping to protect the body from infections, manage inflammation, and respond to allergens and cancer cells.
Disorders of White Blood Cells
| Disorder | Description | Symptoms |
| Leukopenia | Decreased WBC count, increasing infection risk. | Frequent infections, fatigue. |
| Leukocytosis | Increased WBC count, often due to infection or inflammation. | Fever, fatigue, weight loss. |
| Leukemia | Cancer of the blood and bone marrow, characterized by uncontrolled WBC proliferation. | Fatigue, frequent infections, easy bruising. |
Leukopenia results from a variety of conditions, including bone marrow disorders and autoimmune diseases. Leukocytosis is often a response to infection or inflammation but can also indicate leukemia, a serious condition involving uncontrolled WBC growth.
What are Platelets?
Platelets are essential for blood clotting and wound healing. They are cell fragments derived from larger bone marrow cells called megakaryocytes.
Structure and Composition
| Feature | Description |
| Shape | Disk-shaped, non-nucleated cell fragments |
| Origin | Derived from megakaryocytes in the bone marrow |
| Granules | Contain clotting factors and growth factors |
Platelets are not whole cells but are fragments of megakaryocytes, containing granules with proteins essential for clot formation and tissue repair.
Production and Lifespan
| Aspect | Description |
| Production Site | Bone marrow (through thrombopoiesis) |
| Regulation | Hormone thrombopoietin (produced by the liver) |
| Average Lifespan | About 7-10 days |
Platelets are produced in the bone marrow, with their production regulated by thrombopoietin. They have a relatively short lifespan compared to other blood cells.
Functions of Platelets
| Function | Description |
| Hemostasis | Form a platelet plug at injury sites to prevent bleeding. |
| Blood Clot Formation | Activate the clotting cascade to form a stable blood clot. |
| Wound Healing | Release growth factors to aid in tissue repair and regeneration. |
Platelets are crucial for initiating the clotting process to stop bleeding and promoting wound healing through the release of growth factors.
Disorders of Platelets
| Disorder | Description | Symptoms |
| Thrombocytopenia | Low platelet count, leading to bleeding and bruising. | Easy bruising, prolonged bleeding. |
| Thrombocytosis | High platelet count, increasing the risk of clot formation. | Headaches, dizziness, risk of clotting disorders. |
| Hemophilia | Genetic disorder affecting blood clotting factors. | Excessive bleeding, easy bruising, joint pain. |
Thrombocytopenia can result from conditions like leukemia, immune disorders, or bone marrow disorders. Thrombocytosis can be primary (essential thrombocythemia) or secondary (due to inflammation or iron deficiency). Hemophilia is a genetic disorder where blood fails to clot properly due to missing clotting factors.
Types of Blood Cells – FAQs
Q1. What are the primary functions of Red Blood Cells (RBCs)?
Answer: RBCs are primarily responsible for transporting oxygen from the lungs to the body's tissues and carrying carbon dioxide from the tissues back to the lungs for exhalation. They also help in maintaining the pH balance of the blood.
Q2. How are White Blood Cells (WBCs) classified?
Answer: WBCs are classified into two main categories:
Granulocytes: Include neutrophils, eosinophils, and basophils, characterized by granules in their cytoplasm.
Agranulocytes: Include lymphocytes (B cells, T cells, and NK cells) and monocytes, which lack granules.
Q3. What is the role of platelets in blood clotting?
Answer: Platelets play a crucial role in blood clotting by forming a platelet plug at the site of blood vessel injury and activating the clotting cascade to form a stable blood clot. They also release growth factors that aid in tissue repair.
Q4. How is the production of RBCs regulated?
Answer: The production of RBCs, or erythropoiesis, is regulated by erythropoietin, a hormone produced by the kidneys. Erythropoietin is released in response to low oxygen levels in the blood and stimulates the bone marrow to produce more RBCs.
Q5. What are common disorders associated with RBCs?
Answer: Common disorders related to RBCs include anemia (reduced RBC count or hemoglobin), which can lead to fatigue and weakness, and polycythemia (increased RBC count), which can increase the risk of blood clots.
Q6. What functions do neutrophils, eosinophils, and basophils serve?
Answer:
Neutrophils: Act as the first responders to bacterial infections and engage in phagocytosis.
Eosinophils: Combat parasitic infections and are involved in allergic reactions.
Basophils: Release histamine and heparin, playing a role in inflammatory responses and allergies.
Q7. What is the difference between thrombocytopenia and thrombocytosis?
Answer:
Thrombocytopenia: Refers to a low platelet count, which can lead to excessive bleeding and easy bruising.
Thrombocytosis: Refers to a high platelet count, which can increase the risk of abnormal blood clotting and related complications.
Q8. How are WBC disorders such as leukopenia and leukemia diagnosed?
Answer: WBC disorders are typically diagnosed through blood tests and bone marrow examinations.
Leukopenia: Identified by a low WBC count in blood tests, which may indicate infections or bone marrow disorders.
Leukemia: Diagnosed through blood tests showing abnormal WBC counts and the presence of immature cells, as well as bone marrow biopsies.
Q9. How does the lifespan of different blood cells vary?
Answer:
RBCs: Approximately 120 days.
Neutrophils: Few hours to days.
Eosinophils: Few days.
Basophils: Few hours to days.
Lymphocytes: Months to years.
Monocytes: Days to months.
Q10. What role do macrophages play in the immune system?
Answer: Macrophages, which are derived from monocytes, are key players in the immune system. They engulf and digest pathogens, dead cells, and debris through phagocytosis and present antigens to other immune cells to trigger an adaptive immune response.