Acute Coronary Syndrome (ACS) is a term frequently encountered in the realm of cardiology and emergency medicine. It encompasses a range of conditions associated with sudden, reduced blood flow to the heart, leading to various degrees of heart injury or discomfort. Understanding ACS is crucial for healthcare professionals and patients alike, as it plays a significant role in diagnosing and managing heart-related emergencies. This comprehensive guide delves into the full form of ACS, its various types, diagnostic methods, treatment options, and preventive strategies.
What is Acute Coronary Syndrome (ACS)?
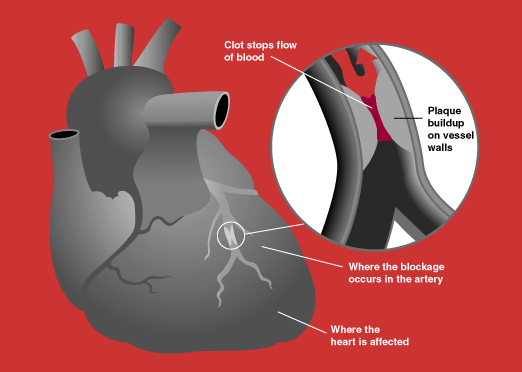
Acute Coronary Syndrome (ACS) is a spectrum of conditions resulting from a sudden reduction or blockage of blood flow to the heart muscle, which can lead to heart tissue damage. ACS is often a result of atherosclerosis, where fatty deposits (plaques) build up in the coronary arteries, causing them to narrow and restrict blood flow. This can ultimately lead to the rupture of a plaque, triggering a clot that obstructs blood flow, causing ischemia or damage to the heart muscle.
- ACS encompasses various clinical manifestations of coronary artery disease.
- It is a medical emergency requiring prompt diagnosis and treatment to minimize heart damage.
Types of ACS
ACS is categorized into three primary types based on the extent and nature of heart muscle damage:
Unstable Angina
Unstable Angina is characterized by sudden, severe chest pain that occurs unpredictably, often at rest. Unlike stable angina, which is triggered by exertion and relieved by rest or medication, unstable angina does not follow a predictable pattern and may not respond to conventional treatments. It signifies a high risk of progression to a more severe form of ACS.
Characteristics:
- Occurs unpredictably and may last longer.
- Pain may not be relieved by rest or nitroglycerin.
- May indicate impending myocardial infarction.
Non-ST-Elevation Myocardial Infarction (NSTEMI)
NSTEMI occurs when a coronary artery is partially blocked, leading to a reduction in blood flow and oxygen to the heart muscle but not complete obstruction. The heart muscle experiences damage, which can be detected through elevated cardiac biomarkers in the blood. NSTEMI does not show significant changes in the ST segment of the ECG.
Characteristics:
Partial blockage of coronary artery.
Elevated cardiac biomarkers (e.g., troponins).
No significant ST-segment elevation on ECG.
ST-Elevation Myocardial Infarction (STEMI)
STEMI is the most severe type of ACS and involves a complete blockage of a coronary artery. This results in significant damage to the heart muscle due to the prolonged lack of blood flow. STEMI is characterized by a significant elevation in the ST segment on the ECG, indicating severe ischemia.
Characteristics:
Complete blockage of coronary artery.
Significant ST-segment elevation on ECG.
Extensive damage to heart muscle.
Causes and Risk Factors
Several factors contribute to the development of ACS, including lifestyle choices, genetic predispositions, and underlying health conditions. The primary causes and risk factors include:
Causes
- Atherosclerosis: Buildup of fatty plaques in the coronary arteries.
- Thrombosis: Formation of blood clots that obstruct blood flow.
- Vasospasm: Sudden constriction of coronary arteries.
Risk Factors
- Age: Increasing age is associated with higher risk.
- Gender: Men have a higher risk at a younger age, while women’s risk increases post-menopause.
- Family History: A family history of heart disease increases susceptibility.
- Smoking: Tobacco use accelerates atherosclerosis.
- Hypertension: High blood pressure damages arterial walls.
- Diabetes: Increases the risk of atherosclerosis and coronary artery disease.
- High Cholesterol: Elevated levels of LDL cholesterol contribute to plaque formation.
- Obesity: Excess weight exacerbates other risk factors.
- Sedentary Lifestyle: Lack of physical activity contributes to cardiovascular issues.
Symptoms of ACS
Recognizing the symptoms of ACS is crucial for timely intervention. Common symptoms include:
- Chest Pain: Often described as pressure, squeezing, or discomfort in the chest, which may radiate to the arms, neck, jaw, or back.
- Shortness of Breath: May occur with or without chest pain.
- Nausea or Vomiting: Some individuals experience gastrointestinal discomfort.
- Sweating: Excessive sweating or cold sweat may occur.
- Fatigue: Unusual fatigue or weakness, especially in women.
- Dizziness or Lightheadedness: Feeling faint or dizzy can be a symptom.
Note: Symptoms may vary between individuals and can be less pronounced in women and elderly patients.
Diagnosis of ACS
Diagnosing ACS involves a combination of clinical evaluation, laboratory tests, and imaging studies to assess heart function and identify the extent of damage.
Clinical Evaluation
A thorough medical history and physical examination are conducted to assess symptoms and risk factors. The clinician will evaluate the pattern, duration, and severity of chest pain and other associated symptoms.
Electrocardiogram (ECG)
An ECG records the electrical activity of the heart and helps identify abnormalities associated with ACS, such as ST-segment elevation or depression.
ECG Findings:
- ST-Elevation: Indicative of STEMI.
- ST-Depression: May suggest NSTEMI or unstable angina.
- T-Wave Inversion: Can be a sign of ischemia.
Blood Tests
Blood tests are essential for measuring cardiac biomarkers that indicate heart muscle damage. Key biomarkers include:
Troponins: Proteins released when heart muscle cells are damaged.
Creatine Kinase-MB (CK-MB): An enzyme found in heart muscle.
Myoglobin: A protein released into the blood after muscle injury.
Imaging Studies
Imaging studies, such as echocardiography and coronary angiography, provide detailed views of heart function and the coronary arteries.
- Echocardiography: Uses ultrasound to visualize heart chambers and assess function.
- Coronary Angiography: An invasive procedure using contrast dye to view blood flow in coronary arteries.
Treatment and Management
Effective management of ACS requires a multidisciplinary approach to restore blood flow, reduce heart damage, and prevent complications.
Medications
Medications play a crucial role in managing ACS. Commonly prescribed drugs include:
- Antiplatelet Agents: Prevent clot formation (e.g., aspirin, clopidogrel).
- Anticoagulants: Prevent blood clots (e.g., heparin).
- Thrombolytics: Dissolve existing clots (e.g., tissue plasminogen activator).
- Beta-Blockers: Reduce heart workload and oxygen demand.
- ACE Inhibitors: Lower blood pressure and prevent heart failure.
- Statins: Lower cholesterol levels and stabilize plaques.
Interventional Procedures
In some cases, interventional procedures may be required to restore blood flow:
- Angioplasty and Stenting: Balloon angioplasty opens blocked arteries, and stents are inserted to keep them open.
- Coronary Artery Bypass Grafting (CABG): Surgery to create a bypass around blocked arteries using grafts.
Lifestyle Changes
Long-term management includes lifestyle modifications to reduce recurrence risk:
- Diet: Adoption of a heart-healthy diet low in saturated fats and cholesterol.
- Exercise: Regular physical activity to improve cardiovascular health.
- Smoking Cessation: Quitting smoking to reduce risk.
- Weight Management: Maintaining a healthy weight.
Preventive Measures
Preventing ACS involves addressing risk factors and adopting a healthy lifestyle. Key strategies include:
- Regular Check-Ups: Monitoring blood pressure, cholesterol levels, and blood sugar.
- Healthy Diet: Consuming a balanced diet rich in fruits, vegetables, and whole grains.
- Physical Activity: Engaging in regular exercise to maintain cardiovascular health.
- Avoiding Tobacco: Refraining from smoking and using tobacco products.
- Managing Stress: Implementing stress-reduction techniques and managing emotional health.
Prognosis and Follow-Up Care
The prognosis for ACS varies based on the severity of the condition and the timeliness of treatment. With appropriate intervention, many individuals can recover and lead healthy lives. Follow-up care is essential for monitoring recovery, managing risk factors, and preventing complications.
Follow-Up Care Includes
- Regular Cardiovascular Check-Ups: Monitoring heart health and function.
- Medication Adherence: Ensuring compliance with prescribed medications.
- Rehabilitation Programs: Participating in cardiac rehabilitation to improve cardiovascular fitness.
Acute Coronary Syndrome (ACS) is a serious and potentially life-threatening condition that requires immediate medical attention. Understanding the types of ACS, recognizing symptoms, and knowing the diagnostic and treatment options are crucial for effective management. By addressing risk factors, adopting a healthy lifestyle, and following medical advice, individuals can significantly reduce their risk of ACS and improve their overall cardiovascular health.
What is Acute Coronary Syndrome (ACS) FAQs
1. What is Acute Coronary Syndrome (ACS)?
Acute Coronary Syndrome (ACS) is a term used to describe a range of conditions caused by a sudden reduction or blockage of blood flow to the heart muscle. This can result in various degrees of heart damage and includes three main types: unstable angina, Non-ST-Elevation Myocardial Infarction (NSTEMI), and ST-Elevation Myocardial Infarction (STEMI). ACS requires prompt medical attention to minimize heart damage and improve outcomes.
2. What are the main symptoms of ACS?
Common symptoms of ACS include chest pain or discomfort (often described as pressure or squeezing) that may radiate to the arms, neck, jaw, or back. Other symptoms can include shortness of breath, nausea or vomiting, excessive sweating, fatigue, and dizziness or lightheadedness. Symptoms can vary among individuals and may be less pronounced in women and the elderly.
3. How is ACS diagnosed?
ACS is diagnosed through a combination of clinical evaluation, electrocardiogram (ECG), blood tests, and imaging studies. A thorough medical history and physical examination are conducted, followed by an ECG to detect heart abnormalities. Blood tests measure cardiac biomarkers like troponins and CK-MB to assess heart muscle damage. Imaging studies, such as echocardiography and coronary angiography, provide detailed views of heart function and coronary arteries.
4. What treatments are available for ACS?
Treatment for ACS includes medications, interventional procedures, and lifestyle changes. Medications may include antiplatelet agents, anticoagulants, thrombolytics, beta-blockers, ACE inhibitors, and statins. Interventional procedures, such as angioplasty and stenting or coronary artery bypass grafting (CABG), may be necessary to restore blood flow. Lifestyle changes, including adopting a heart-healthy diet, engaging in regular exercise, and managing risk factors, are also important for long-term management.
5. How can ACS be prevented?
Preventing ACS involves addressing risk factors and adopting a healthy lifestyle. Key preventive measures include regular cardiovascular check-ups, maintaining a healthy diet, engaging in regular physical activity, quitting smoking, managing stress, and controlling conditions like hypertension, diabetes, and high cholesterol. By making these lifestyle changes and following medical advice, individuals can significantly reduce their risk of developing ACS.